Lupus Rash vs Rosacea: What’s the Difference?
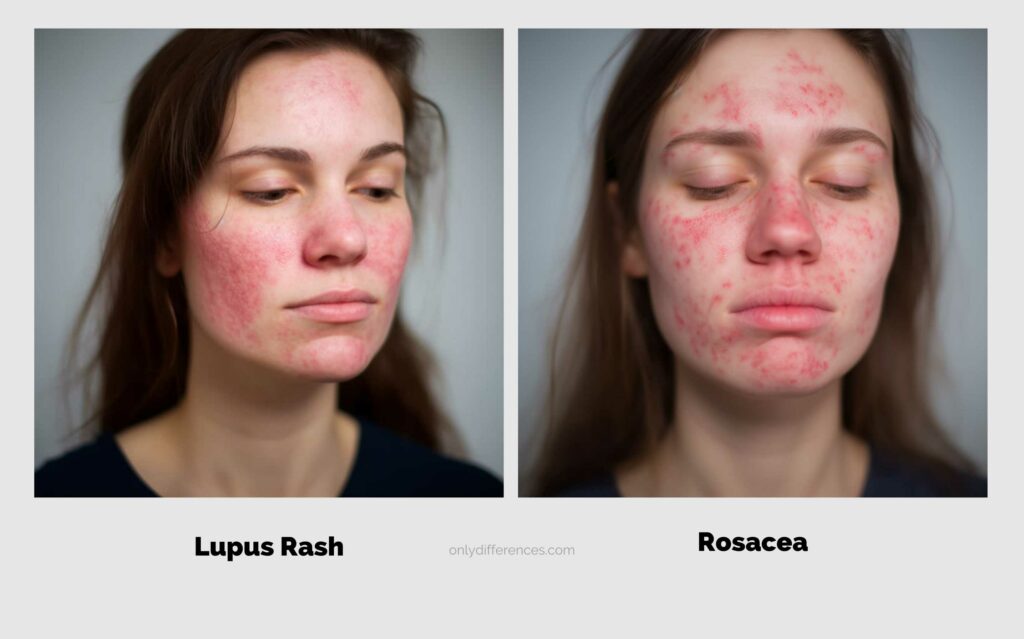
While both lupus rash and rosacea cause facial redness, lupus rash often occurs in a butterfly pattern, and it is associated with a systemic autoimmune disease, whereas rosacea primarily causes persistent redness in the central face, visible blood vessels and acne-like bumps without systemic symptoms.
This article aims to delve deeper into these conditions, helping readers understand the key differences between Lupus Rash vs Rosacea.
Table of Contents
Introduction: Lupus Rash and Rosacea
Skin conditions often serve as outward signs of our internal health. Lupus rash and Rosacea often confound patients and healthcare providers among the myriad dermatological conditions.
Although these two conditions share features like redness and inflammation, they are fundamentally different, originating from distinct underlying causes and manifesting different symptomatology.
Lupus Rash
Systemic lupus erythematosus, or simply lupus, is a chronic autoimmune disease. In these cases, the immune system mistakenly attacks healthy tissues, including the skin, resulting in various symptoms.
One of the most common and recognizable manifestations of lupus is the so-called ‘butterfly’ rash, also known as a malar rash. This rash spans across the cheeks and nose, resembling a butterfly’s wings, and affects roughly 50% of those with lupus.
The lupus rash is usually flat or slightly raised, with a red, and sometimes scaly, appearance. It’s important to note that while it is most commonly seen on the face, it can occur anywhere on the body. In discoid lupus, which affects only the skin, circular, disk-shaped lesions can appear on the scalp, face, and ears.
Other lupus symptoms can accompany the rash, including fatigue, joint pain, fever, and sensitivity to light. It’s worth noting that the rash can flare up in response to sun exposure, stress, or no apparent cause at all, similar to the systemic flares seen in lupus.
Rosacea
On the other hand, Rosacea is a chronic skin condition characterized by persistent facial redness, flushing, and, in some cases, acne-like bumps. It typically affects adults over 30, especially those with fair skin, and it is believed to be caused by a combination of hereditary and environmental factors.
Rosacea primarily impacts the central face, encompassing the cheeks, nose, forehead, and chin. The redness, which can come and go, is often accompanied by visible blood vessels and small, red, pus-filled bumps.
Unlike lupus rash, rosacea does not cause systemic symptoms like joint pain or fever. It can, however, be associated with ocular symptoms like dryness, irritation, and swollen, reddened eyelids, a condition known as ocular rosacea.
It’s interesting to note that certain triggers can exacerbate Rosacea, such as spicy foods, alcohol, temperature extremes, stress, and sun exposure. Therefore, managing these triggers plays a crucial role in controlling Rosacea’s progression.

Differentiating Factors: Lupus Rash vs Rosacea
While both conditions may appear similar due to the characteristic redness, several key factors differentiate a Lupus rash from Rosacea.
- Age and Demographics: Lupus typically presents in younger women of childbearing age (15-44 years), while Rosacea is common in individuals aged 30 to 50, with a slight preference for women.
- The pattern of Skin Involvement: The malar or ‘butterfly’ rash of lupus is quite distinctive, spreading over the cheeks and the bridge of the nose. While also affecting the central face, Rosacea often extends to the forehead and chin, which are generally spared in lupus.
- Associated Symptoms: While lupus is a systemic disease associated with fatigue, fever, joint pains, and photosensitivity, Rosacea is limited to the skin and eyes without systemic manifestations.
- Skin Lesions: Lupus rashes are often flat or slightly raised and can be scaly. In contrast, Rosacea frequently presents with red bumps, pimples, and visible blood vessels.
- Response to Sun Exposure: Both conditions can flare with sunlight, but photosensitivity is more associated with lupus. UV light can trigger a systemic response in lupus, not just a localized skin reaction.
Differences between lupus rash and rosacea
| Lupus Rash | Rosacea | |
|---|---|---|
| Age | Common in younger women of childbearing age (15-44 years) | Common in adults aged 30 to 50 |
| Demographics | Affects both sexes, but more prevalent in women | Affects both sexes, but more common in women, especially those with fair skin |
| Skin Involvement | Characteristic ‘butterfly’ rash spreading over cheeks and bridge of the nose | Persistent redness on the central face, extending to the forehead and chin |
| Associated Symptoms | Fatigue, fever, joint pains, photosensitivity | Limited to skin and eyes, no systemic manifestations |
| Skin Lesions | Flat or slightly raised, sometimes scaly rash | Red bumps, pimples, visible blood vessels |
| Response to Sun Exposure | Can trigger a systemic response, not just a localized skin reaction | Can exacerbate the condition, but generally causes only localized skin reaction |
Are lupus rash and rosacea hereditary?
Both lupus rash and rosacea have been found to have a genetic component, but they are not directly inherited in a simple pattern. Having a family member with lupus or rosacea can increase your risk of developing the condition, but environmental factors also play a significant role.
Therefore, while genetics can contribute to susceptibility, they do not guarantee that you will develop either lupus rash or rosacea.
How can lupus rash and rosacea affect one’s quality of life?
Lupus rash and rosacea conditions lead to skin changes that can be a source of self-consciousness and psychological distress. This can impact social interactions, professional opportunities, and overall mental well-being. Some individuals may experience depression, anxiety, and lower self-esteem as a result.
Specifically for lupus, beyond the rash, the systemic involvement can cause fatigue, joint pain, and other symptoms that interfere with daily activities and physical function. Flares can be unpredictable, adding to the stress and making planning difficult.
With rosacea, symptoms like persistent facial redness, visible blood vessels, and pimple-like bumps can lead to embarrassment or social anxiety. In addition, ocular rosacea can cause discomfort and vision problems, further impacting quality of life. The chronic nature of rosacea, with periods of flare-ups and remission, can also be stressful and disruptive.
Although both conditions can be challenging, effective management can mitigate these impacts. This includes not only medical treatments but also psychological and emotional support, patient education, and lifestyle adaptations to manage triggers and symptoms.
What kind of specialist should I see for lupus rash and rosacea?
For both lupus rash and rosacea, a dermatologist – a doctor specializing in conditions of the skin – is the primary healthcare provider you should consult. Dermatologists have the expertise to diagnose and manage various skin conditions, including these.
However, since lupus is a systemic disease that can affect various parts of the body beyond the skin, you may also need to see a rheumatologist, a specialist in autoimmune diseases.
On the other hand, if rosacea symptoms extend to your eyes (a condition known as ocular rosacea), seeing an ophthalmologist would be beneficial. Additionally, given that both lupus and rosacea can have psychological impacts due to their visible nature and chronic course, consulting a mental health professional like a psychologist or psychiatrist may be beneficial for holistic care.
Are the treatments for lupus rash and rosacea the same?
The treatments for lupus rash and rosacea are not the same, reflecting the distinct underlying pathologies of these conditions.
Treatment options for lupus rash often include anti-inflammatory drugs like nonsteroidal anti-inflammatory drugs (NSAIDs), antimalarial drugs like hydroxychloroquine, corticosteroids, and immunosuppressants. For skin-specific symptoms, topical corticosteroids and sunscreens are typically recommended.
On the other hand, rosacea’s treatment focuses on controlling the symptoms and may include topical treatments to reduce redness and inflammation, such as metronidazole, azelaic acid, or ivermectin. Oral antibiotics like tetracyclines may be used for their anti-inflammatory properties. In cases where rosacea results in visible blood vessels or thickened skin, laser treatments or surgery may be options.
Lifestyle modifications such as avoiding triggers, sun protection, and a skin-friendly diet can complement medical treatments for both conditions.
Nevertheless, the fundamental differences in these conditions make it crucial to consult a healthcare provider for an accurate diagnosis and treatment plan.
Can children develop lupus rash or rosacea?
Children can develop lupus rash and rosacea, though it is less common than adults. Childhood lupus is a serious condition and often more aggressive than lupus in adults, with the rash being one of its manifestations.
Rosacea, on the other hand, is exceedingly rare in children. When it does occur in this age group, it’s often misdiagnosed due to its rarity.
Regardless, if a child presents with symptoms of either condition, prompt evaluation by a healthcare provider is necessary.
Can stress trigger a lupus rash or rosacea flare-up?
In lupus, stress can stimulate the immune system, potentially leading to increased inflammation and a subsequent flare-up of symptoms, including the characteristic rash. It’s worth noting that managing stress is a critical part of the overall strategy for controlling lupus, as stress can impact the rash and other symptoms.
Similarly, in rosacea, emotional stress is a well-known trigger for flare-ups. Stress can cause dilation of blood vessels, leading to flushing and redness associated with rosacea. Furthermore, the skin’s barrier function can be disrupted under stress, potentially worsening rosacea symptoms.
Therefore, stress management, including strategies like regular exercise, meditation, deep breathing exercises, and maintaining a good sleep schedule, plays a crucial role in managing both conditions. It’s important to remember that while managing stress can help control symptoms, it’s not a substitute for medical treatment.
Conclusion: Lupus Rash vs Rosacea
While Lupus rash and Rosacea can cause facial redness and discomfort, understanding their differences is key to accurate diagnosis and effective treatment. If you suspect you have either of these conditions, it’s essential to consult a dermatologist or rheumatologist who can conduct a comprehensive examination and recommend appropriate treatment.
Everyone’s experience with Lupus and Rosacea is unique, and what works for one person may not work for another. Listen to your body, and don’t be afraid to seek medical advice when necessary. Skin health, after all, is an integral part of our overall well-being.
References
- Blount, B. Wayne, and Allen L. Pelletier. “Rosacea: a common, yet commonly overlooked, condition.” American family physician.
- Weinstein, C., et al. “Lupus and non‐lupus cutaneous manifestations in systemic lupus erythematosus.” Australian and New Zealand journal of medicine.
- Zhao, Raymond, Severine Cao, and Frank Wang. “Facial rash with exuberant crusting in pregnancy.” International Journal of Women’s Dermatology.
Read more articles
